What is PsA?
What is PsA?
In PsA, the body’s immune system attacks its own joints
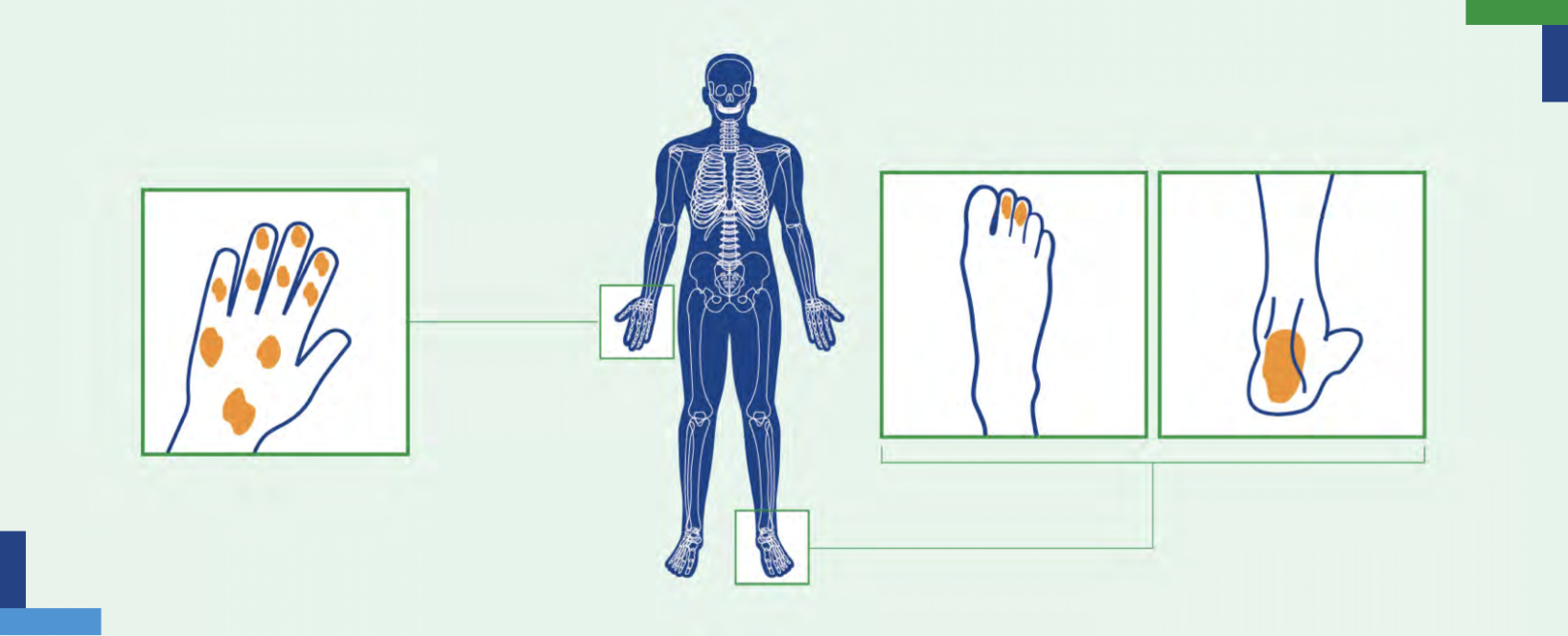
How psoriatic arthritis affects the body4
About 80% of people with PsA also have skin psoriasis, but they don’t always develop at the same time56
Neither PsA nor psoriasis (Pso) is contagious,78 but it can mean that you stand a greater risk of developing some other disease, such as diabetes, cardiovascular disease, inflammatory intestinal disease, auto-immune eye disease, fibromyalgia or depression.9
You maybe be interested in

Make every moment of the consultation really count.

Does psoriatic arthritis (PsA) always stay the same?

You’re not alone – there are other patients with psoriatic arthritis, just like you out there.
* The immune system is a complex set of cells and molecules designed to defend the body against foreign substances including cancer cells, toxins and parasites. When the system turns towards body (so-called `self`) components, immune-mediated inflammatory diseases occur. Examples of these are rheumatoid arthritis, psoriasis, psoriatic arthritis and multiple sclerosis.10